What is a Clinical Audit and Why Should You Do It?


Your Electronic Health Record (EHR) system can help make your practice more efficient. A clinical audit NextGen report is one tool that you can use to get the most out of your EHR investment. A clinical audit will show you gaps, bottlenecks, and emerging issues in your appointment, coding, and documentation workflows. Here is what you need to know about EHR clinical audits.
How a Clinical Audit Can Help Your Practice
EHRs do not just organize and manage patient data; they also gather and store a wealth of information about your practice patterns. A clinical audit aggregates and displays key metrics about your practice's patient visit workflows. It can help you identify bottlenecks and emerging issues in with your patient appointments. For example, TempDev's NextGen EHR Clinical Audit Report helps you keep track of vital patient visit data in real-time to keep your practice on track.
A clinical audit shows you data about appointments and the data charted in the Practice Management and EHR system. Key measures include the following:
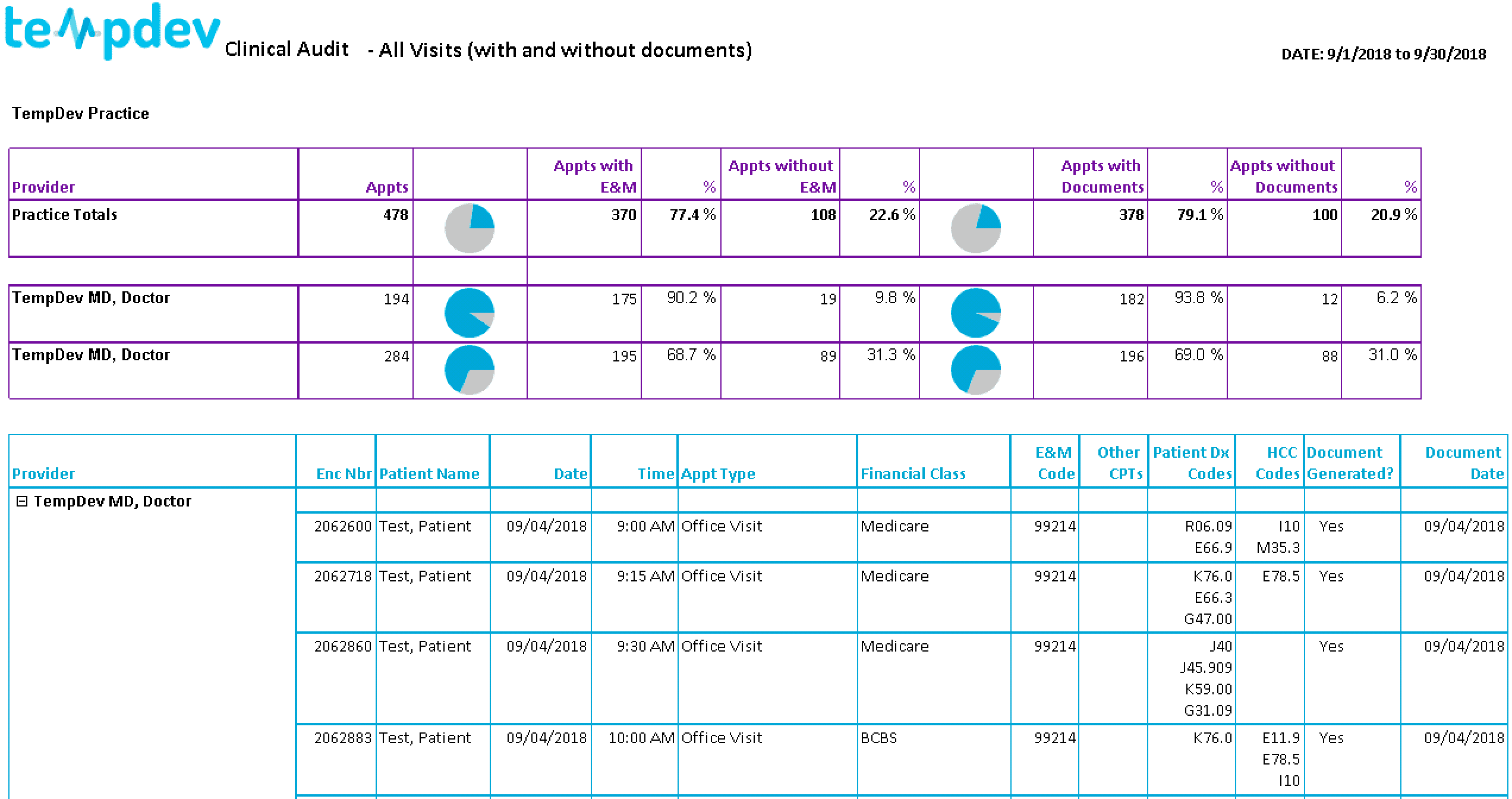
The total number of appointments, overall and by physician
The share of appointments that have an Evaluation and Management (E&M) code, overall and by physician
The share of appointments that have documentation, overall and by physician
The patient's primary financial class
Patient diagnoses and HCCs
Documentation generated
In an office-based practice, most visits should include E&M codes. By tracking the share of appointments with E&M codes, you can gauge the quality of visit coding. E&M codes also indicate whether the appointment was with a new or established patient. If providers are consistently using appropriate E&M codes, a clinical audit can also provide information on the share of appointments for new versus established patients.
A clinical audit will also show you the share of appointments with documentation. With proper EHR use, every patient visit should generate a chart note or other documentation. If many appointments have no documentation, providers may not be using the EHR system effectively and billing may not want to charge for the visit. Additionally, a lack of documentation can increase your practice's audit risk. Tracking visit documentation can help you identify audit risks or problems with EHR use before they become critical issues.
You can also view clinical audit metrics by the provider or by the patient. The provider view can help you determine if some providers are struggling with coding, documentation, or EHR use. The patient view shows details on patients' insurance type, diagnosis codes, and HCC codes, if applicable. These patient-level details can help you assess the thoroughness of documentation, and they can help you find potential gaps in diagnosis coding.
Using Clinical Audits to Analyze and Improve Workflows
A clinical audit can show you gaps in appointment coding and documentation. Proper coding and documentation of appointments are critical to ensure full reimbursement. Also, missing documentation can create audit risks for your practice. By tracking clinical audit metrics, your practice can identify and fix workflow issues that cause incomplete coding or documentation. This will both increase your efficiency and improve reimbursement.
If your practice has many appointments missing documentation or E&M codes, that may signal that providers are struggling with the EHR system or are facing time pressure from appointment scheduling. Your practice could address these issues with EHR training or better appointment scheduling. By finding and addressing these issues as they arise, you can save time and money.
Clinical audits can also identify providers who are seeing fewer patients, struggling with coding, or documenting appointments less frequently than their peers. By comparing appointment metrics across providers, you can target training and workflow interventions where they are most needed. You can also see how patients' financial classes vary across providers. A provider with a large number of Medicare patients may need different training on coding and documentation than a provider with a large number of privately insured patients, for example.
Implementing a Clinical Audit in NextGen EHR
Conducting a clinical audit in your EHR system is simple and straightforward with the right NextGen EHR reporting tools. Your EHR gathers a wealth of data about your practice and your appointments, and NextGen reports and dashboards can help you access and aggregate that information quickly and easily. With a properly-configured clinical audit report template, you can track key metrics about your practice in real-time.
TempDev's NextGen EHR Clinical Audit Report will gather and display all the data you need to conduct a clinical audit. TempDev can also customize the tool to fit your practice's needs. With the Clinical Audit Report, you can assess your practice's appointment workflows, identify bottlenecks, and make adjustments to fix problems before they become entrenched. Clinical audits focus on appointment coding and documentation, helping you ensure that critical reimbursement tasks are being completed timely.
How TempDev Can Help
TempDev's consultants are NextGen EHR experts. TempDev can help you conduct clinical audits in your NextGen EHR.
Call us at 888.TEMP.DEV, or contact us here to get started with NextGen's clinical audit tools.
Interested?
Agree with our point of view? Become our client!
Did you enjoy this read? Feel free to share it with your contacts.






