Related articles:
What Healthcare Leaders Should Expect From a Strong PMO Partner
Read ArticleIntroducing Ryan White 3.0 Reporting
Read ArticleWhy Healthcare IT Projects Need a Project Manager Before the Work Begins
Read ArticleOur new MIPS Executive Summary is a high-level summary that highlights the most important information you need to know for successful reporting this year.
Are you ready for MIPS or do you feel a little confused about the process? Don’t worry if you don’t feel ready, TempDev has your back! As a part of our ongoing commitment to our clients on MACRA, we’ve created a MIPS Executive Summary that will walk you through some of the more difficult to understand details of the QPP and what you need to do for reporting.
In the summary, we look at what makes up the MIPS Composite Performance Score and why you need to report at least something for this year, even if your practice isn’t fully prepared for meeting the reporting requirements. This year’s reporting will affect your 2019 payments significantly. For instance, if you don’t participate in the reporting at all, you will receive a negative 4% payment adjustment for the 2019 payment year. Meanwhile, if you submit at least some data, you’ll avoid a negative payment adjustment. The more data you report, the better off you’ll be. If you report even just ninety days worth of data, you’ll earn a neutral or even a small positive payment adjustment. Of course, submitting data for the full year is the best option, as it will earn you a much larger positive payment adjustment. As such, not reporting for 2017 can have a severely detrimental effect on your 2019 Medicare payments.
We review the technical requirements clients need to meet for transitional year (2017) and 2018 reporting. It's critical to your MIPS success to understand which version of NextGen EHR you need to be on and when in order to meet the MIPS requirements. Developing a budget and timeline, along with securing any resources needed for this upgrade is vital to achieving the highest MIPS scores possible.
In the MIPS Deep Dive section of the Executive Summary, we look at the four categories that make up MIPS reporting. As you may know, the MIPS track is combining three current Medicare programs and adding a fourth category, Clinical Practice Improvement Activities (CPIA). In this new system, Advancing Care Information (ACI) is taking over Meaningful Use (MU), Quality Measures are replacing Physician Quality Report System (PQRS), and Resource Use (Cost) is taking the place of Value Based Modifier (VBM).
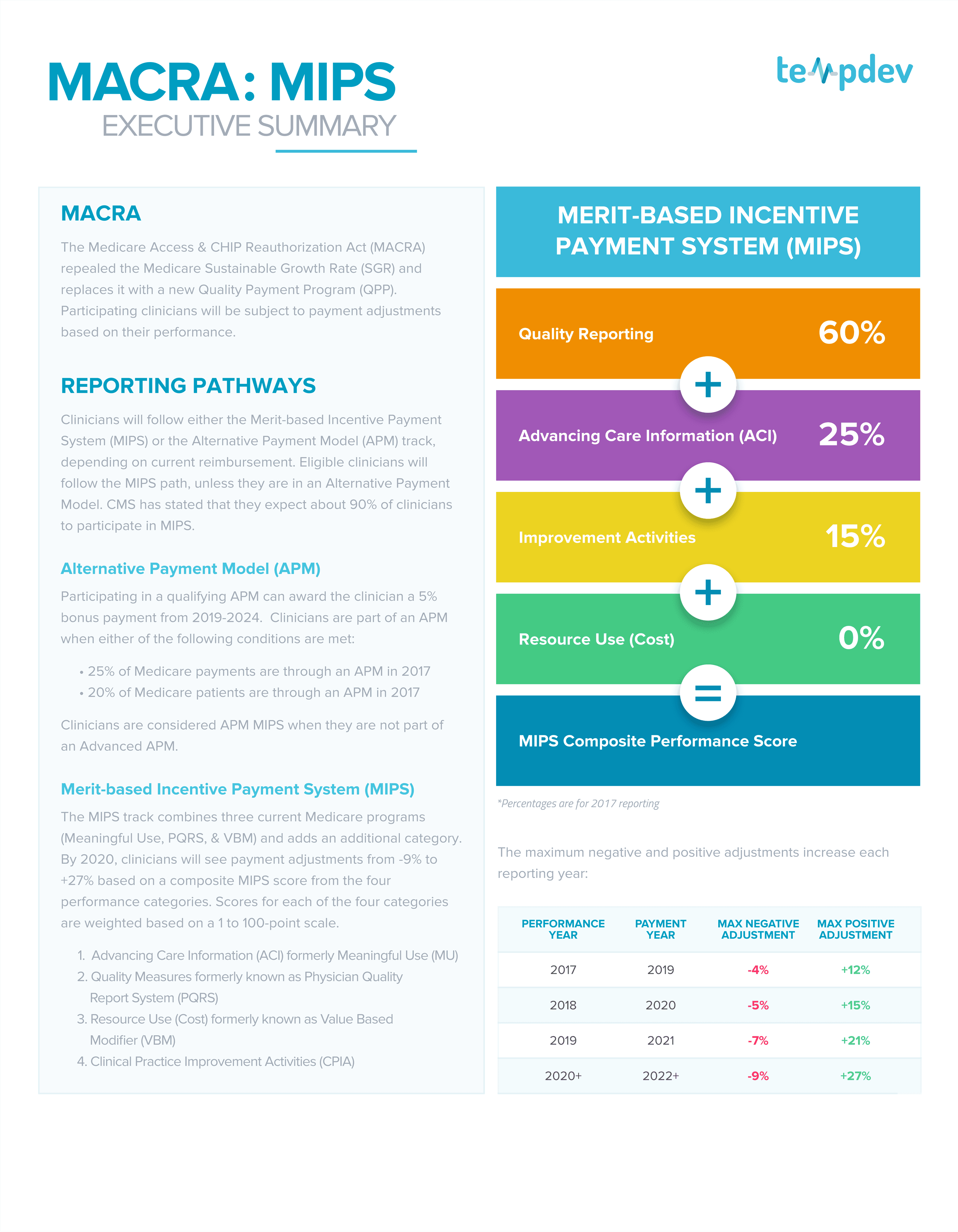
The scores for each of the four categories are weighted based on a 100 point scale. Quality Measures comprises up 60% of your score, while ACI is 25% and Improvement Activities comprises 15%. This year, cost data is collected from informational claims and will not have any impact on the overall composite score. Each category has several different measure sets available for reporting. In our MIPS Deep Dive we also explain each category and examples for how to meet the measures in the category.
MACRA
The Medicare Access & CHIP Reauthorization Act (MACRA) repealed the Medicare Sustainable Growth Rate (SGR) and replaces it with a new Quality Payment Program (QPP). Participating clinicians will be subject to payment adjustments based on their performance. Clinicians will follow either the Merit-based Incentive Payment System (MIPS) or Alternative Payment Model (APM) track depending on current reimbursement.
Reporting Pathways
CMS has stated that they expect about 90% of MACRA clinicians to participate in MIPS. Eligible clinicians will follow the MIPS path unless they are in an Alternative Payment Model (APM).
Alternative Payment Model (APM)
Participating in a qualifying APM can award the clinician a 5% bonus payment from 2019-2024. Clinicians are part of an APM when either of the following conditions are met:
25% of Medicare payments are through an APM in 2017
20% of Medicare patients are through an APM in 2017
Clinicians are considered APM MIPS when they are not part of an Advanced APM.
Merit-based Incentive Payment System (MIPS)
The MIPS track combines three current Medicare programs (Meaningful Use, PQRS, & VBM) and adds an additional category. By 2020, clinicians will see payment adjustments from -9% to +27% based on a composite MIPS score from the four performance categories. Scores for each of the four categories are weighted based on a 1 to 100-point scale.
Advanced Care Information (ACI) formerly Meaningful Use (MU)
Quality Measures formerly known as Physician Quality Report System (PQRS)
Resource Use (Cost) formerly known as Value Based Modifier (VBM)
Clinical Practice Improvement Activities (CPIA)
MIPS Payments
Your MIPS Composite Performance Score will be based on the following:
Quality Reporting - 60%
Advancing Care Information (ACI) - 15%
Improvement Activities - 15%
Resource Use (Cost) - 0%
The maximum negative and positive adjustments increase each reporting year:
Technical Requirements
Successful MACRA MIPS reporting requires the following:
NextGen Regulatory Release (version 5.9/KBM 8.4) recommended upgrade in early 2018 (required by October 1, 2018). The application and KBM upgrade are performed at the same time. *
NextGen Patient Portal or a patient portal solution
NextGen Share
NextGen HQM
NextGen Care, NextGen Population Health, or another population health solution is recommended
*Pending release of MACRA 2018 Final Rule from CMS
Eligible Clinicians
The following clinicians are eligible for 2017 and 2018 reporting:
Physicians (MD/DO and DMD/DDS)
Physician Assistants
Nurse Practitioners
Clinical Nurse Specialists
Certified Registered Nurse Anesthetists
Exempt Clinicians
Select clinicians and facilities are exempt from the MIPS program:
First year Medicare participants
Below low volume threshold
Less than $30k in allowed Medicare charges
Less than 100 Medicare patients seen in a year
Participating in Medicaid Meaningful Use
They will still need to upgrade by January 1, 2018 to participate in Meaningful Use Stage 3 and includes FQHCs, CHCs, and Planned Parenthood.
Exempt but may be eligible after 2019:
Physical Therapists
Occupational Therapists
Speech Language Pathologists
Audiologists
Certified Nurse Midwives
Clinical Social Workers
Clinical Psychologists
Dietitians/Nutritional Professionals
2017 MIPS Reporting Options
Clinicians are offered the following four MIPS reporting options for 2017:
Don't Participate - The clinician will receive a negative 4% payment adjustment if no data is submitted for 2017.
Submit Something - The clinician will avoid a negative payment adjustment if some data is submitted (ex: one QM and one ACI).
Submit a Partial Year - The clinician will earn a neutral or small positive payment adjustment if 90 days of data is submitted.
Submit a Full Year - The clinician will earn a positive payment adjustment if a full year of 2017 data is submitted.
Group vs Individual Reporting
MIPS participants must decide to report either as a group or an individual.
When reporting as a group, all encounters are reported based on the tax ID number. Therefore, all encounters are reported together, regardless of the clinician.
When reporting as an individual, encounters are reported based on the clinician’s NPI
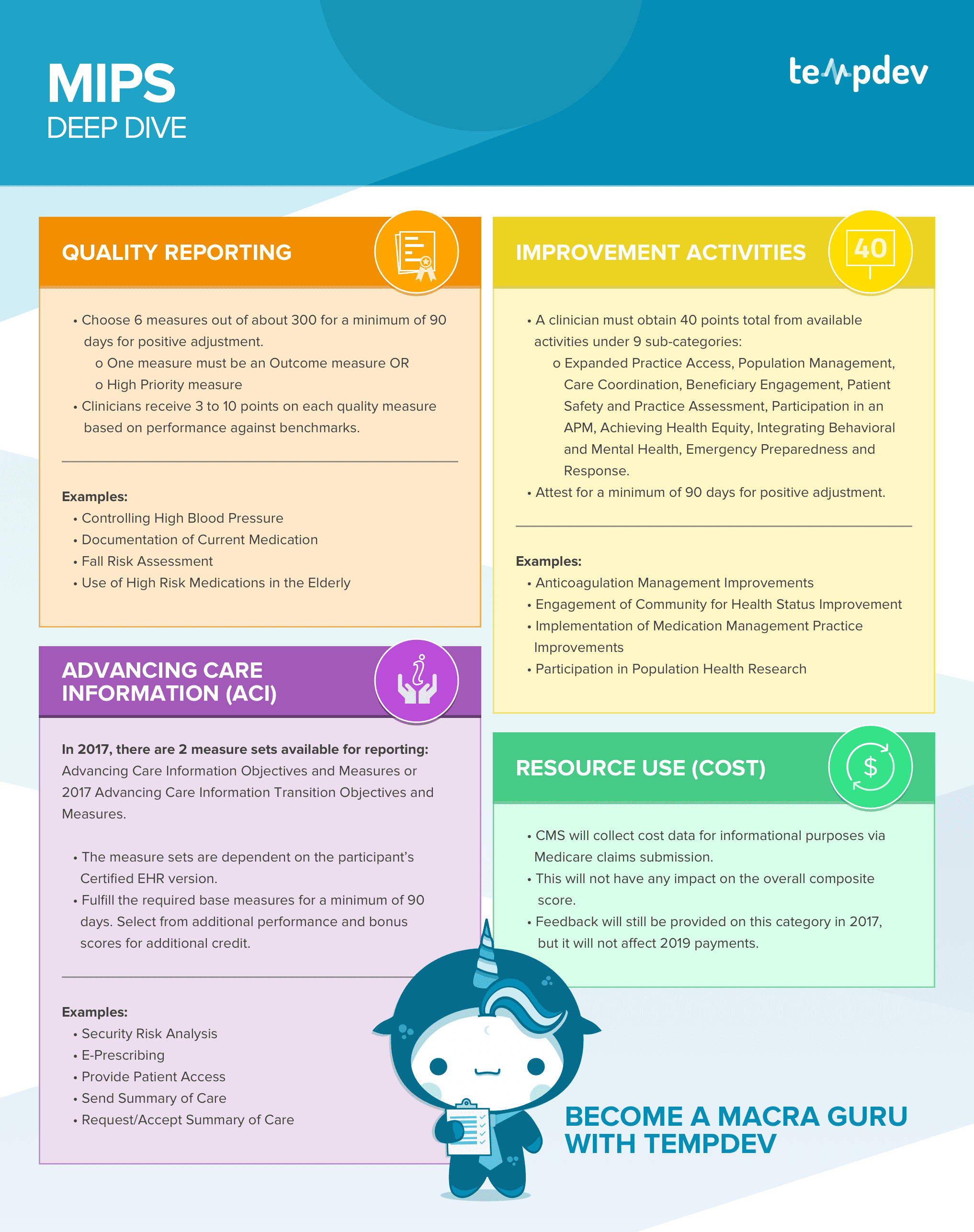
MIPS Deep Dive
Quality Reporting
Choose 6 measures out of about 300 for a minimum of 90 days for positive adjustment
One measure must be an Outcome measure OR High Priority measure
Clinicians receive 3 to 10 points on each quality measure based on performance against benchmarks
Examples:
Controlling High Blood Pressure
Documentation of Current Medication
Fall Risk Assessment
Use of High Risk Medications in the Elderly
Advancing Care Information (ACI)
In 2017 there are 2 measure sets available for reporting Advancing Care Information Objectives and Measures or 2017 Advancing Care Information Transition Objective and Measures:
The measure sets are dependent on the participant's Certified EHR version.
Fulfill the required base measures for a minimum of 90 days. Select from additional performance and bonus scores for additional credit.
Examples:
Security Risk Analysis
E-Prescribing
Provide Patient Access
Send Summary of Care
Request/Accept Summary of Care
Improvement Activities
A clinician must obtain 40 points total from available activities under 9 sub-categories:
Expanded Practice Access
Population Management
Care Coordination
Beneficiary Engagement
Patient Safety and Practice Assessment
Participation in an APM
Achieving Health Equity
Integrating Behavioral and Mental Health
Emergency Preparedness and Response
Attest for a minimum of 90 days for a positive adjustment.
Examples:
Anticoagulation Management Improvements
Engagement of Community for Health Status Improvement
Implementation of Medication Management Practice Improvements
Participation in Population Health Research
Resource Use (Cost)
CMS will collect cost data for informational purposes via Medicare claims submission.
This will not have any impact on the overall composite score.
Feedback will still be provided on this category in 2017 but will not affect 2019 payments.
Getting Started
Here are your first steps to planning your transition to MACRA:
Determine your MACRA path: MIPS, APM MIPS, or Advanced APM
Develop a MACRA road map and timeline for the next two years
Work on getting organizational buy-in
Create an upgrade budget and allocate resources
Decide whether to report as a group or individual clinician
Review the TempDev MIPS Toolkit
Contact us to plan your successful MACRA transition
Contact us to partner with our expert level TempDev MACRA consultants to create a more detailed implementation plan that will cater to your unique business needs!


Interested?
Agree with our point of view? Become our client!
Did you enjoy this read? Feel free to share it with your contacts.








